The Systems Behavioral Health Practices Need for a Sustainable Hybrid Care Model
Key Takeaways
- Hybrid care is now the default care model, with in-person and virtual visits operating side by side as part of routine delivery.
- Seamless hybrid care depends on consistent workflows for scheduling, intake, documentation, communication, and payments—regardless of visit format.
- Most operational strain comes from disconnected systems and modality-specific exceptions, not from hybrid care itself.
- Practices scale hybrid care successfully by standardizing workflows, reducing manual handoffs, and keeping systems aligned around a single visit record.
- PracticeQ provides the unified operational platform that allows practices to deliver, manage, and scale hybrid care from one system.
Six years after the pandemic, hybrid care is no longer an experiment. For behavioral health and modern care practices, in-person and virtual visits now function as a single, permanent care model.
As a result, your practice is expected to work across both physical and virtual settings at once, with core systems staying connected regardless of how care is delivered.
In this blog, we walk through what it takes to support that model seamlessly, and how to keep operations steady as expectations, volume, and complexity continue to rise.
What Is Hybrid Care—and Why It’s Now the Standard
Hybrid care is a care delivery model in which in-person and virtual visits are planned, supported, and managed through the same operational systems.
In other words, the mechanics around care don’t change based on where a visit happens. The same systems support scheduling, intake, documentation, billing, and follow-up across both in-person and virtual care.
That consistency is important because care no longer lives in a single, physical setting: In behavioral health, 67% of encounters now happen virtually.
At that scale, hybrid care isn’t a configuration choice. It’s the baseline most practices are already being held to, whether their systems are built for it or not.
Where Hybrid Care Breaks Down for Most Practices
Hybrid care can add complexity to your day, especially when the systems you rely on aren’t fully aligned. In many practices, virtual and in-person visits may still be supported by separate tools, rules, and workflows.
When that happens, small gaps can start to show up. Instead of one clear process your team can rely on, staff may find themselves managing exceptions as they go. Over time, those small fixes can stack up and quietly become part of the daily routine.
Here are some areas practices feel the strain first.
Fragmented Scheduling Across Visit Types
Scheduling is often one of the first places friction can surface. A visit may be booked, but the details behind it still need attention.
- Providers appear available without the correct room or telehealth setup
- Appointments require manual adjustment after booking to align space, links, or coverage
- Schedule changes don’t carry through across systems
- Appointments are rescheduled once conflicts are uncovered
When the schedule doesn’t reflect what a visit actually requires, staff can’t rely on it at face value. They check, confirm, and adjust throughout the day to keep things running smoothly. That added work increases operational load and makes scheduling less dependable over time.
Disconnected Intake and Documentation
Intake and documentation are another common pressure point in hybrid environments. Forms, consent, and charting often follow different workflows depending on visit type.
- Patients receive different forms for virtual and in-person visits
- Consent is collected through multiple workflows
- Intake information lives across systems or documents
- Staff manually confirm whether intake is complete
Without a consistent intake process, sessions start with uncertainty. Staff spend time tracking down information and fixing gaps before care begins, which slows the day down and adds unnecessary stress for both staff and patients.
Inconsistent Payments and Follow-ups
Billing and follow-ups can also be affected when workflows aren’t connected.
- Charges post late because visit details aren’t fully synchronized
- Payments require manual reconciliation across tools
- Follow-up messages and reminders go out inconsistently
- Patients contact the practice with questions about unclear or delayed bills
When these issues come up, payments can take longer to resolve, and staff end up spending more time answering billing questions. And for patients, the whole process can be confusing and hard to follow.
What “Seamless” Hybrid Care Actually Requires
Seamless hybrid care comes down to operational continuity. When a visit can change formats without creating extra work, your workflows are doing their job. Here’s what has to stay consistent: scheduling, intake, and patient communication.
One Scheduling Experience for All Visit Types
Scheduling is the control center for hybrid care. If your schedule doesn’t carry the right visit details at booking, everything downstream becomes manual.
To keep scheduling reliable across in-person and telehealth, you need the visit setup to be decided once and reflected everywhere.
That means your scheduling workflow should:
- Treat visit type as the source of truth. Each visit type should define duration, modality options, location requirements, and any rules tied to that service.
- Match availability to the actual modality. Providers shouldn’t appear bookable for virtual if they’re only seeing patients in person during that block, and vice versa.
- Assign the right resources automatically. In-person bookings should include room assignment as part of booking, not as a separate step later.
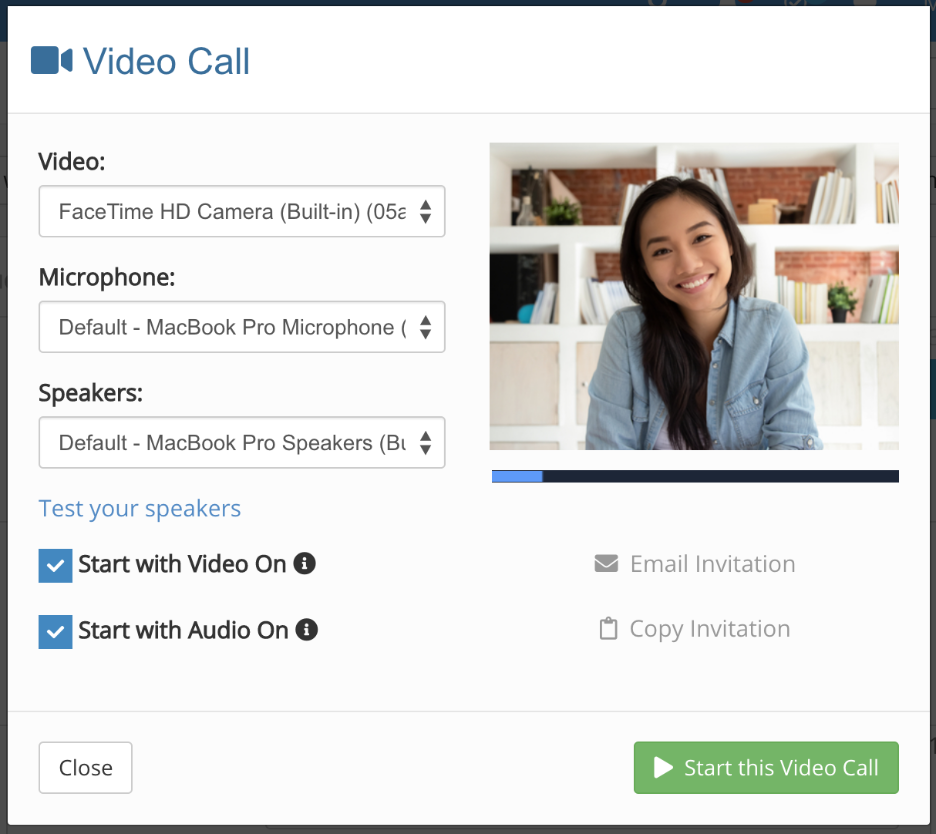
- Generate telehealth details at booking. The link should be created, stored, and available in the same place staff and patients already look.
- Handle changes without rebuilds. If a patient switches from in-person to virtual, staff shouldn’t need to create a new appointment, resend a chain of messages, or manually update multiple systems.
A simple pressure test: take a scheduled in-person appointment and switch it to virtual. If staff have to touch more than the appointment itself to make it real, scheduling isn’t unified yet.
Standardized Intake and Consent Workflows
Hybrid care falls apart when intake depends on delivery method. Patients don’t care what system you use. They just want to know what to do, where to do it, and to not be asked for the same information twice.
Standardized intake means the practice collects the right information the same way every time for a given service, regardless of whether the session is virtual or in person.
To get there:
- Build intake around visit type, not modality. Start with what’s required for the service (history, screening tools, policies, financial agreements) and keep it consistent.
- Package forms and disclosures into a single flow. Patients should receive one clear set of steps, not a mix of links, PDFs, and follow-up emails.
- Capture consent once, store it once. Consent should live in the patient record with a timestamp and be easy to confirm without digging.
- Make intake status visible before the session. Staff should be able to see “complete” versus “missing” at a glance and know exactly what’s missing.
- Avoid re-entry. Intake data should land where it’s used, not sit in a separate tool that forces staff to copy and paste into the chart.
Operationally, this is the goal: sessions start on time with the right information already in place, instead of staff using the first five minutes to hunt down forms or confirm consent.
Unified Patient Engagement and Communication
For patients, hybrid care is defined by how and when they hear from your practice. If messaging changes based on visit format, patients get mixed signals, staff get more inbound questions, and small mistakes turn into no-shows or late starts.
Focus on making three moments predictable:
Before the visit
- Send reminders on a consistent cadence.
- Include the right details by default: location for in-person visits, join link for virtual visits, plus any prep steps.
- Keep rescheduling and cancellation options clear and easy.
At visit time
- Make check-in simple and consistent.
- If a visit is virtual, the patient shouldn’t have to search across emails or texts for the link.
After the visit
- Follow-up should run the same way across modalities: next steps, scheduling prompts, forms, payment requests, and any resources the patient needs.
When engagement is unified, patients get clear, consistent direction at every step. Plus, staff spend less time untangling messages and more time supporting care.
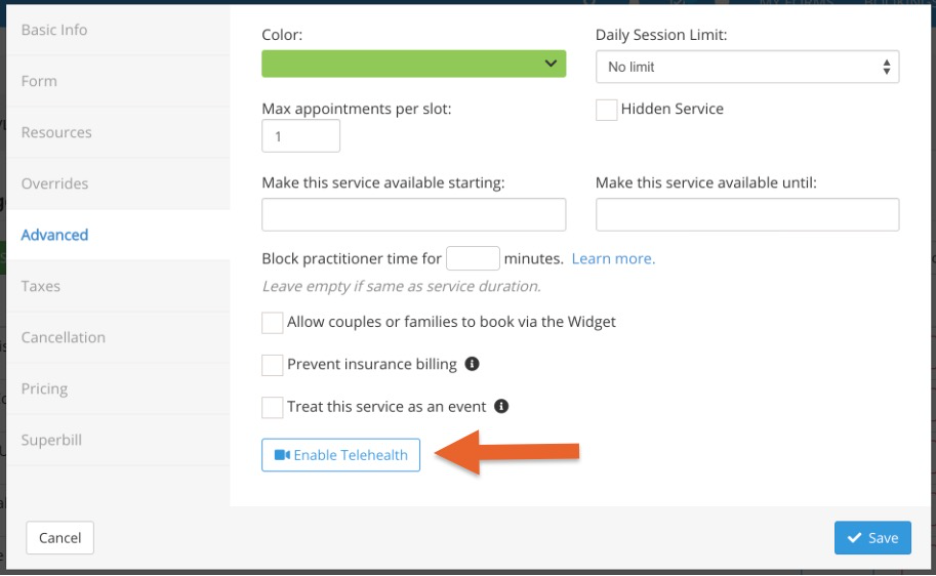
Operational Workflows That Support Hybrid Care at Scale
Hybrid care is only successful if core workflows function the same way across in-person and virtual visits. Here’s how practices do that without adding operational overhead.
Documentation That Works Across Modalities
Documentation needs to follow the visit, not the format. Clinicians shouldn’t change how they chart based on whether care happens in person or over video.
To support hybrid care at scale, documentation workflows should:
- Use consistent note templates based on service, not modality
- Pull visit context automatically from the schedule, including provider, duration, and visit type
- Carry intake data and screening tools directly into the chart
- Support the same completion and signing process for all visits
AI-assisted notes can help reduce documentation time, especially in behavioral health, as long as they fit into the same workflow clinicians already use. Notes should be easy to review, edit, and finalize without creating a separate process for virtual care.
When documentation works this way, clinicians spend less time charting and staff don’t have to reconcile notes across systems.
Payments That Don’t Care Where Care Happens
Billing should behave the same way every time a visit is completed. The modality shouldn’t introduce special handling, side rules, or cleanup work.
In a scalable hybrid setup, payment workflows are driven by the visit record itself:
- Charges generate from completed appointments and signed notes
- Visit type and payer logic determine billing behavior automatically
- Patient balances live in a single ledger
- Statements, payment links, and reminders follow one process
- Changes to the appointment update billing without manual fixes
The goal is a payment flow that doesn’t require staff to pause and think about how care was delivered before they move forward.
Integrated Systems That Reduce Manual Work
To scale hybrid care, teams need systems that stay in sync around each visit. Otherwise, staff end up reconciling records across tools just to keep things aligned.
That means:
- Appointment data flows directly into documentation and billing
- Patient details, insurance, and consent stay in sync
- Signed notes feed reporting and financial workflows automatically
- Payment activity updates balances and follow-ups without rework
Any step that requires copying information from one system to another becomes a scaling problem fast.
Compliance Considerations for Hybrid Care Delivery
Hybrid care introduces new compliance considerations in behavioral health. Care often includes crisis assessment, highly sensitive disclosures, minors or guardians, and in some cases, substance use treatment records. Strong compliance practices help protect both patients and care teams.
Consistency is the most effective safeguard. When workflows are aligned across in-person and virtual care, teams are less likely to miss key steps and more able to deliver care with confidence.
Patient Consent and Documentation Standards
Consent and documentation should work reliably across visit types without relying on staff memory or manual workarounds.
For most behavioral health practices, this includes:
- Using an informed consent that clearly covers telehealth
- Keeping consent status current and easy to locate in the patient record
- Avoiding separate consents unless regulations require them
That also means documentation should follow a consistent structure for every visit. For virtual care, ensure notes capture:
- Modality of care
- Patient location
- Emergency contact confirmation
- Who was present
- Any technical issues that affected care
Embedding these elements into note templates helps maintain accuracy and completeness.
Privacy and Secure Communication
Patients trust your practice with more than what they say in session. Messages, forms, and reminders carry that same responsibility.
At a minimum:
- Use HIPAA-aligned telehealth and messaging tools
- Limit access through role-based permissions and audit logs
- Route protected health information through secure channels by default
When email or text is used, document patient preference and keep content appropriate and limited. For virtual visits, begin with a brief privacy check to confirm the patient’s setting.
Practices treating substance use disorders should also confirm whether 42 CFR Part 2 applies and ensure those requirements are reflected in access and disclosure workflows.
Operational Consistency Reduces Risk
In hybrid care, inconsistent workflows are a common source of compliance issues.
Risk is reduced when practices:
- Standardize intake, consent, and documentation
- Make required fields difficult to skip
- Centralize patient communication
- Define clear escalation paths for crisis language or missed high-risk visits
With predictable workflows, required steps are less likely to be missed.
How Unified Platforms Simplify Hybrid Care
Hybrid care adds pressure to already complex operations. A unified platform brings scheduling, intake, engagement, documentation, and payments into one system, giving teams a reliable way to support care across visit types.
PracticeQ acts as the operational backbone for hybrid behavioral health care:
- Consistent scheduling and intake for virtual and in-person visits
- Integrated telehealth, secure messaging, and documentation
- Billing and payments connected directly to care delivery
- Centralized patient communication and system integrations
With the right foundation, hybrid care becomes easier to manage and easier to sustain.
Start a free PracticeQ trial and run hybrid care from one system.
FAQs
What is hybrid care in healthcare?
Is hybrid care appropriate for behavioral and mental health practices?
What are the biggest challenges of hybrid care delivery?
How do practices keep hybrid care compliant?
Do practices need separate systems for in-person and virtual care?
Behavioral Health Outpaces Primary Care in 2024. (2024). American Hospital Association. https://www.aha.org/aha-center-health-innovation-market-scan/2025-11-11-behavioral-health-outpaces-primary-care-2024
Norton, C. (2025, August 1). The New Standard: Practice Management Software with Built-In Telehealth. PracticeQ. https://www.practiceq.com/resources/practice-management-software-with-telehealth
Schwalbe, D., Sodemann, M., Iachina, M., Bente Mertz Nørgård, Nina Høj Chodkiewicz, & Jette Ammentorp. (2023). Causes of Patient Nonattendance at Medical Appointments: Protocol for a Mixed Methods Study. JMIR Research Protocols, 12, e46227–e46227. https://doi.org/10.2196/46227


